The short answer is: yes, there is a connection between androgens and HS, but it is not as simple as "high testosterone causes HS." Understanding the actual mechanism helps men make informed decisions about their treatment and lifestyle.
Is Testosterone Causing HS?
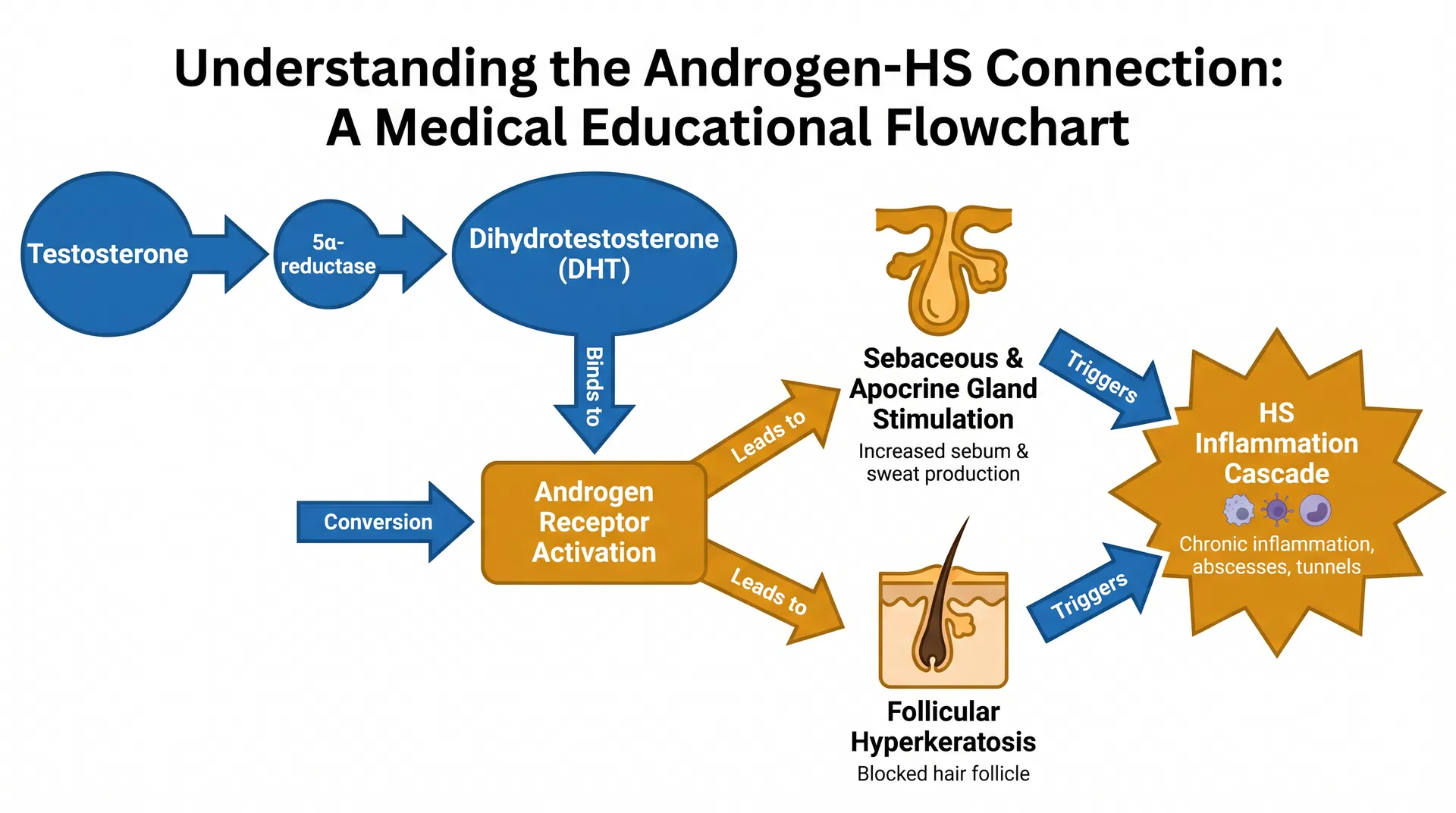
HS is not caused by testosterone alone. It is a chronic inflammatory condition driven by follicular occlusion, immune dysregulation, and genetic factors. But androgens, including testosterone and its derivatives, do play a role in the biology of the glands that HS affects.
The apocrine and sebaceous glands, which are central to HS, are androgen-sensitive. Higher androgen activity can:
- Increase sebum production, contributing to follicular plugging
- Enlarge sebaceous glands, making occlusion more likely
- Stimulate apocrine gland activity, increasing secretion in affected areas
- Promote inflammatory signaling in skin tissue
What Research Suggests
The evidence on androgens and HS is suggestive but not definitive. Key findings from the research:
Anti-androgen treatments help some women with HS
Spironolactone and other anti-androgens reduce HS flares in some female patients, providing indirect evidence that androgen activity contributes to disease activity.
HS can flare with TRT in some men
Case reports document HS onset or worsening after starting testosterone replacement therapy. The mechanism is thought to involve increased androgen stimulation of affected glands.
Most men with HS do not have abnormal testosterone levels
HS is not simply a disease of high testosterone. Androgen receptor sensitivity and local skin metabolism of androgens may be more relevant than serum testosterone levels.
Finasteride has shown benefit in some HS patients
Finasteride, which blocks conversion of testosterone to DHT (a more potent androgen), has been used off-label in HS with mixed results, suggesting DHT may be more relevant than testosterone itself.
Reality Check
Testosterone does not cause HS, and having HS does not mean your testosterone is too high. But if you are considering TRT, anabolic steroids, or testosterone-boosting supplements, discuss the potential impact on your HS with your dermatologist before starting.
Practical Guidance for Men with HS
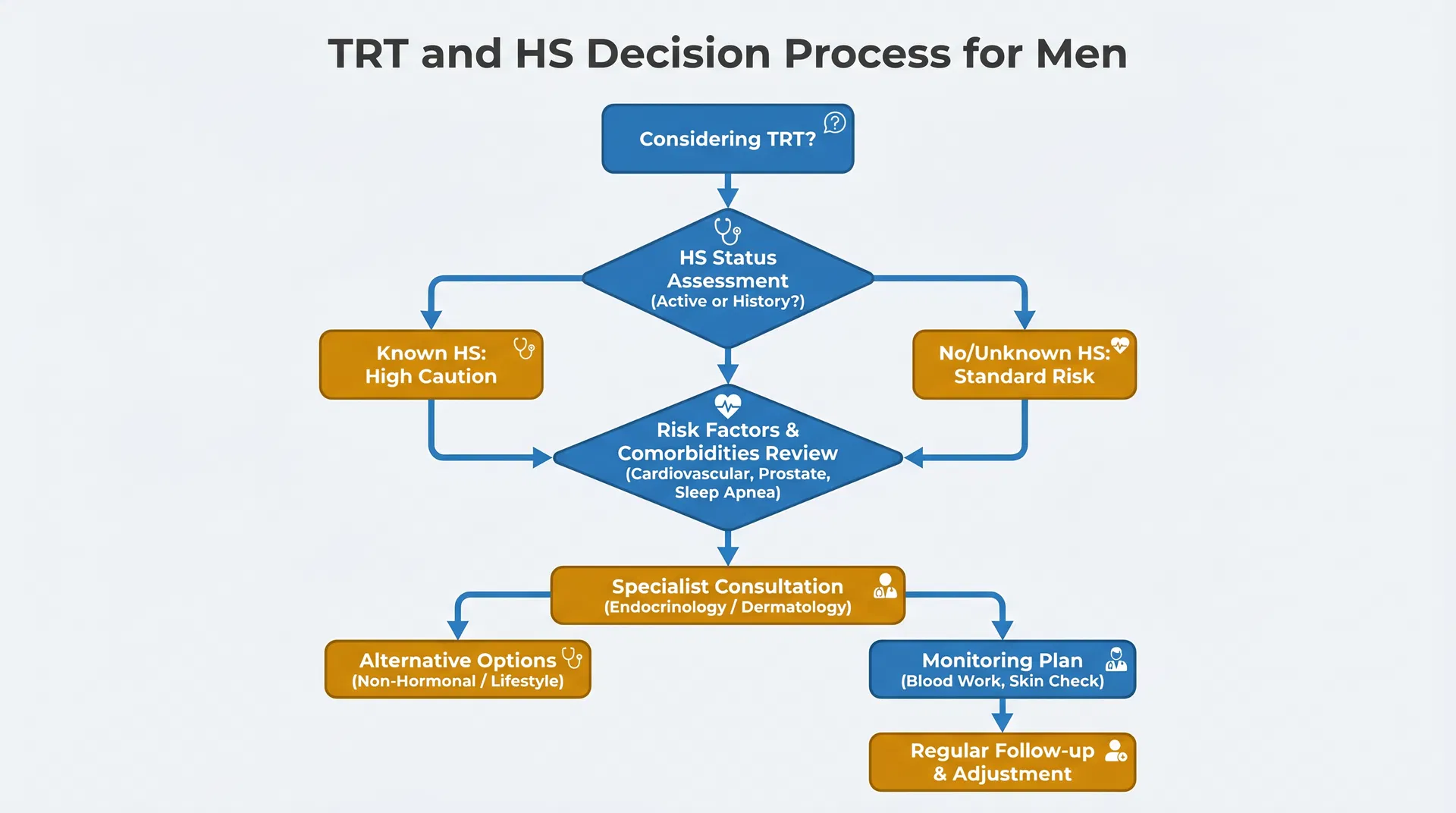
If you are considering TRT
- Discuss HS history with your prescribing doctor
- Start at the lowest effective dose
- Monitor for HS flares in the first 3-6 months
- Have a plan with your dermatologist if HS worsens
If you use anabolic steroids
- Anabolic steroids are a significant HS trigger
- Even short cycles can cause severe flares
- This is one of the most under-reported HS triggers in men
- Discuss honestly with your dermatologist
If you take testosterone boosters
- OTC testosterone boosters vary widely in ingredients
- Some contain compounds that may affect androgen levels
- No strong evidence they worsen HS, but caution is warranted
- Discuss with your doctor if HS is active
Monitoring your HS
- Track flare frequency and location
- Note any changes after starting new supplements
- Report changes to your dermatologist promptly
- Consider a flare diary for pattern recognition
Related Resources
Frequently Asked Questions
This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to hormone therapy or supplements.
References
- [1] Jemec GB. Hidradenitis suppurativa. N Engl J Med. 2012;366(2):158-164.
- [2] Scheinfeld N. Hidradenitis suppurativa: a practical review of possible medical treatments based on over 350 hidradenitis patients. Dermatol Online J. 2013;19(4):1.
- [3] Alikhan A, et al. North American clinical management guidelines for hidradenitis suppurativa. J Am Acad Dermatol. 2019;81(1):76-90.
- [4] Giamarellos-Bourboulis EJ, et al. Complex immunological interactions in hidradenitis suppurativa: a systematic review. J Eur Acad Dermatol Venereol. 2016;30 Suppl 1:9-13.
- [5] Zouboulis CC, et al. European S1 guideline for the treatment of hidradenitis suppurativa/acne inversa. J Eur Acad Dermatol Venereol. 2015;29(4):619-644.