When HS affects the buttocks, it changes how a person sits, moves, works, and sleeps. It is not a minor inconvenience. For many men, it is one of the most disabling aspects of living with HS, and one of the least talked about.
Where HS Shows Up on the Buttocks
HS does not appear randomly. It targets areas with high concentrations of apocrine glands and areas where skin rubs against skin or clothing. On the buttocks, the most common locations are:
- The gluteal fold (the crease between the buttock and upper thigh)
- The intergluteal cleft (between the two buttocks)
- The lower buttocks where skin contacts seating surfaces
- The perianal area (covered in the next article in this series)
Men with HS have significantly higher rates of gluteal involvement than women. Research suggests this is linked to androgen activity, body composition differences, and the tendency for men to delay seeking care until lesions are advanced.
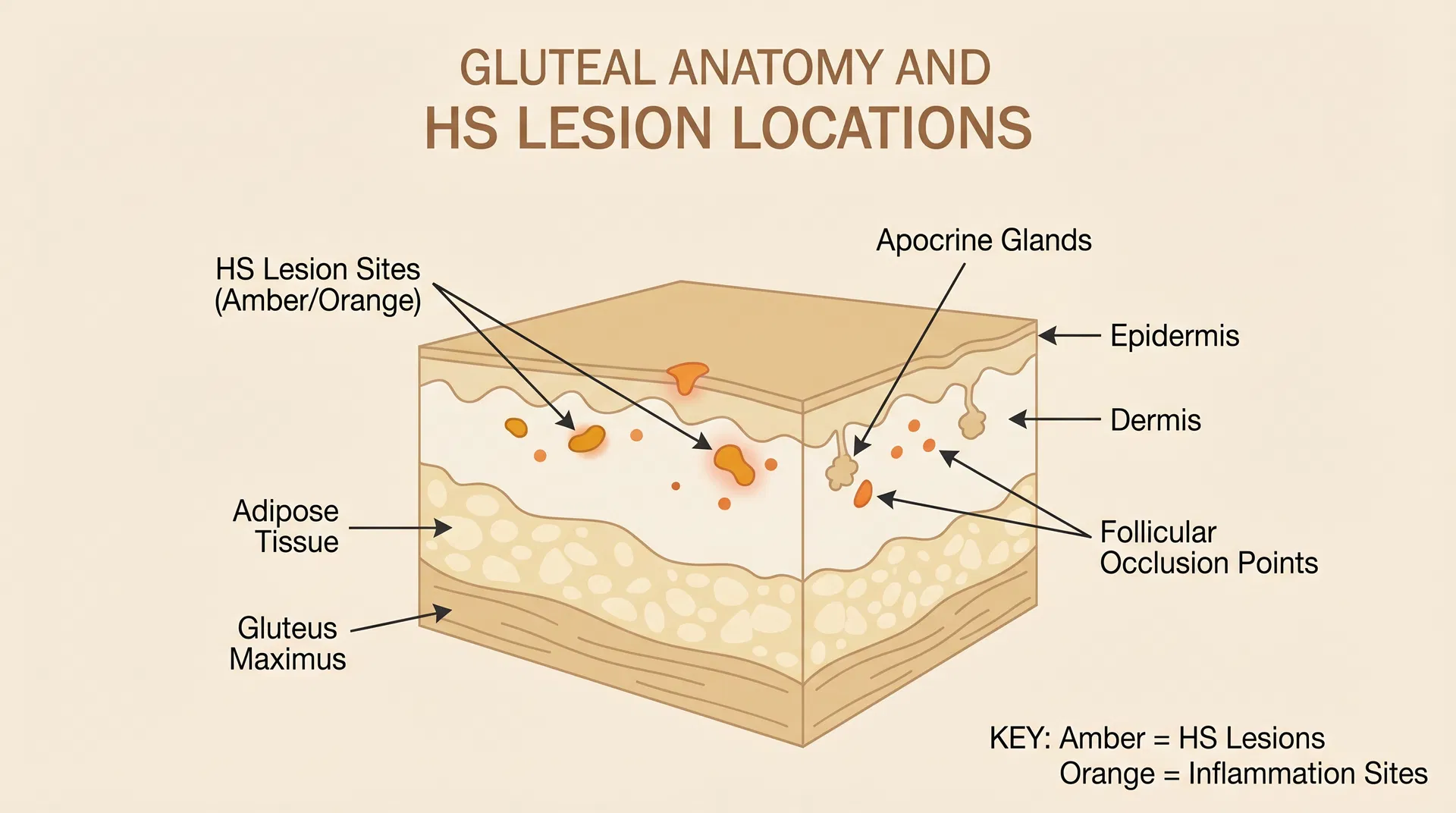
What It Looks Like: Stages of Gluteal HS
Gluteal HS follows the same Hurley staging system as HS elsewhere, but the presentation can be more severe due to constant pressure and friction.
Early (Hurley I)
Single or multiple painful nodules or boils. No tunneling. Often mistaken for ingrown hairs or folliculitis.
Moderate (Hurley II)
Recurring abscesses that drain. Early sinus tract formation. Significant pain when sitting or moving.
Severe (Hurley III)
Extensive tunneling under the skin. Rope-like scarring. Continuous drainage. May involve the entire gluteal region.
Men are more likely to present at Hurley Stage II or III, partly because the gluteal location makes lesions harder to see and easier to dismiss as something minor.
The Biggest Trigger Most Men Overlook
Prolonged sitting is the single most underestimated trigger for gluteal HS flares. Desk workers, drivers, and anyone who sits for more than four hours a day without breaks is at elevated risk of worsening lesions.

Other commonly overlooked triggers include:
- Tight underwear or jeans that create constant friction in the gluteal fold
- Synthetic fabrics that trap heat and moisture
- Shaving or waxing the gluteal area
- High-impact exercise without moisture-wicking clothing
- Obesity or rapid weight changes that alter friction patterns
Reality Check
Gluteal HS is not caused by poor hygiene. Washing more aggressively can actually worsen lesions by disrupting the skin barrier. Gentle cleansing with a fragrance-free, non-comedogenic wash is recommended.
Managing Gluteal HS Day to Day
Seating
- Use a coccyx cutout or donut cushion
- Stand or shift position every 30-60 minutes
- Avoid hard chairs during active flares
Clothing
- Loose-fitting, moisture-wicking underwear (bamboo or cotton)
- Avoid tight jeans or synthetic fabrics
- Seamless underwear reduces friction points
Wound Care
- Gentle cleansing with Hibiclens or fragrance-free wash
- Non-stick dressings for draining lesions
- Change dressings after exercise or sweating
Medical
- Topical clindamycin for early lesions
- Biologics for moderate-severe disease
- Wide local excision for tunneling/scarring
Related Resources
Frequently Asked Questions
This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment of hidradenitis suppurativa.
References
- [1] Jemec GB. Hidradenitis suppurativa. N Engl J Med. 2012;366(2):158-164.
- [2] Alikhan A, et al. North American clinical management guidelines for hidradenitis suppurativa. J Am Acad Dermatol. 2019;81(1):76-90.
- [3] Garg A, et al. Prevalence and co-morbidities of hidradenitis suppurativa in the United States. Dermatology. 2014;228(3):261-265.
- [4] Canoui-Poitrine F, et al. Characteristics of a series of 302 French patients with hidradenitis suppurativa. J Am Acad Dermatol. 2009;61(1):51-57.
- [5] Zouboulis CC, et al. European S1 guideline for the treatment of hidradenitis suppurativa/acne inversa. J Eur Acad Dermatol Venereol. 2015;29(4):619-644.