HS and Men's Mental Health: Shame, Silence, and the Weight No One Talks About
Men with hidradenitis suppurativa carry a psychological burden that rarely gets named. This article addresses it directly.
Part of the Men's HS Series - practical guides written for men with HS
View full seriesHidradenitis suppurativa is a physically painful condition. But for many men, the psychological weight is just as heavy. Shame about lesion location. Silence around a condition that feels too embarrassing to name. Years of misdiagnosis that erode trust in healthcare. Relationships strained by pain, odor, and self-consciousness.
Men with HS are significantly less likely than women to seek mental health support, even when they are experiencing clinical depression or anxiety. This article addresses the psychological burden of HS in men directly, without minimizing it or dressing it up.
The Shame Factor: Why HS Hits Men Differently
Shame is not a side effect of HS. For many men, it is the dominant experience of the disease. The location of lesions in the groin, buttocks, and perianal area creates a specific kind of shame that is hard to articulate and harder to share.
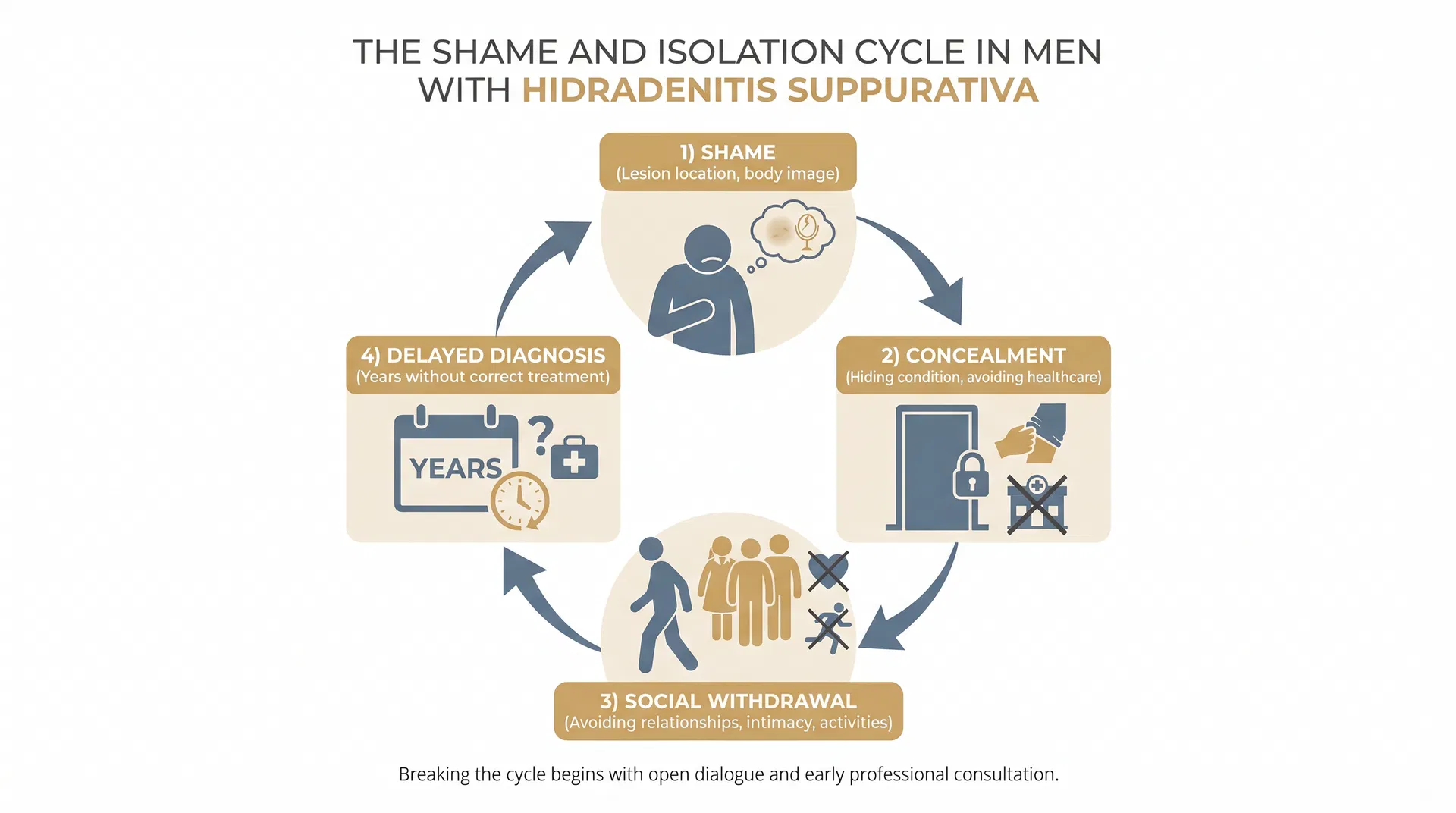
Masculine norms create silence
Social expectations around stoicism and self-sufficiency make it harder for men to acknowledge emotional distress. Many men describe their HS as 'something I just deal with' for years before seeking any kind of support.
Location amplifies shame
Lesions in the groin, inner thighs, buttocks, and perianal area are associated with hygiene and sexuality. Men often fear that healthcare providers or partners will misinterpret the condition as a sexually transmitted infection or a result of poor hygiene.
Isolation compounds the burden
Men are less likely to have peer networks where chronic illness is openly discussed. Women with HS have more access to online communities and support groups. Men often carry the psychological burden alone, which worsens both mental health outcomes and disease management.
Delayed diagnosis extends the wound
The average time from first HS symptom to correct diagnosis is 7 to 10 years. For men, this delay is often longer. Years of being told 'it's just a boil' or 'lose weight' by healthcare providers creates a specific kind of medical trauma that persists even after diagnosis.
What the Research Shows
The psychological burden of HS is not anecdotal. It is well-documented in clinical literature, even if it is underaddressed in clinical practice.
of people with HS meet criteria for depression
Significantly higher than the general population rate of 7-10%
average delay to correct HS diagnosis
Each misdiagnosis year adds to psychological burden and erodes trust
higher risk of anxiety disorders in HS vs. general population
Driven by unpredictability of flares, pain, and social stigma
quality-of-life impairment comparable to psoriasis and rheumatoid arthritis
HS consistently ranks among the highest QoL-impairing dermatological conditions
Importantly, mental health does not automatically improve when HS is treated. Men who have spent years in shame and isolation often need direct psychological support alongside medical treatment to recover their quality of life.
The Delayed Diagnosis Wound
Being told for years that your condition is 'just boils,' 'poor hygiene,' or 'something you should lose weight to fix' is a form of medical invalidation that leaves lasting psychological marks.
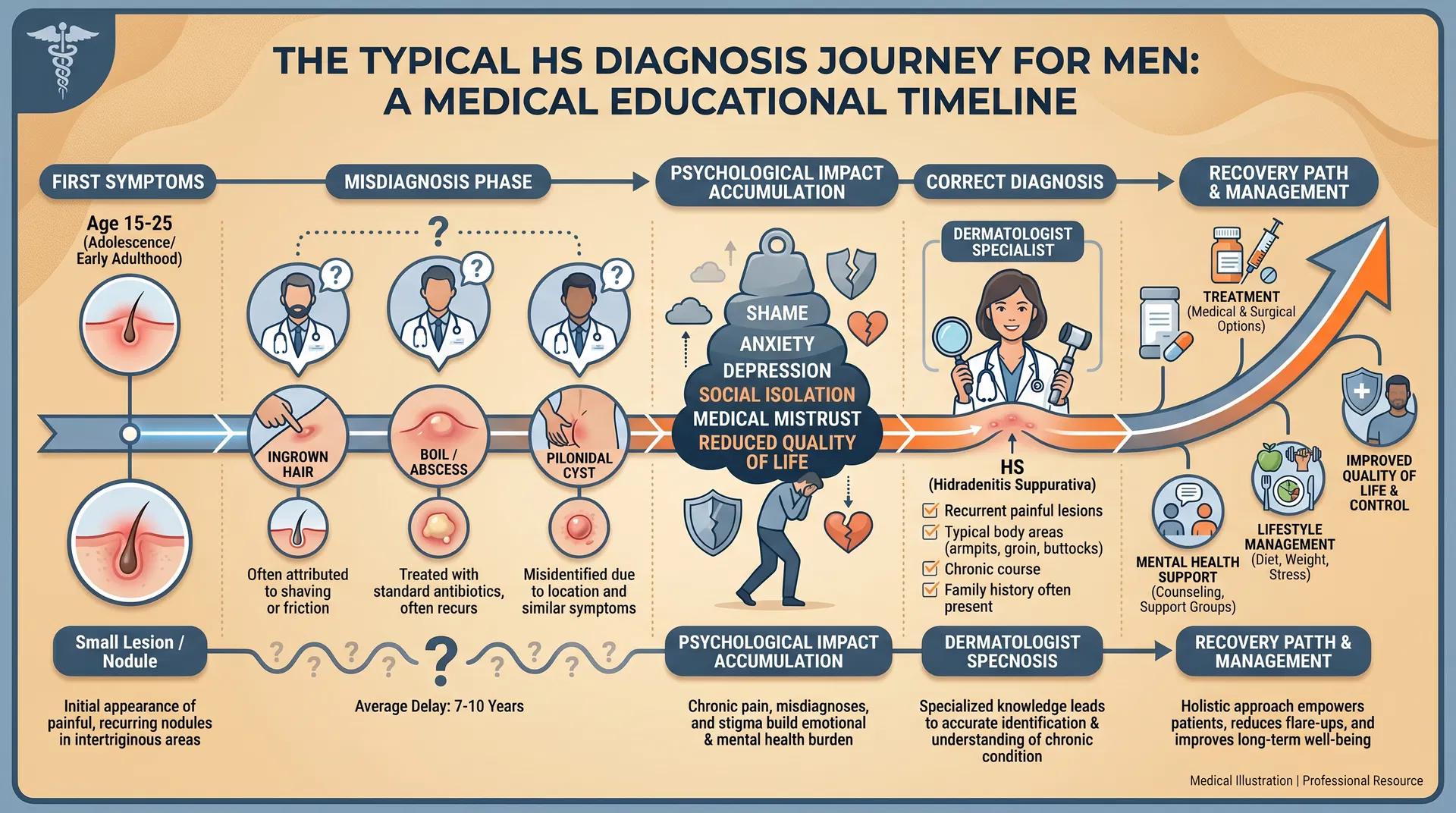
What Men With HS Are Often Told Before Diagnosis
- "It's just an ingrown hair" - repeated for years
- "You need to lose weight" - without any further investigation
- "Keep the area clean" - implying the cause is poor hygiene
- "It's a pilonidal cyst" - treated surgically without addressing the underlying disease
- "Come back if it gets worse" - dismissing the current severity
Each dismissal reinforces the belief that the condition is not real, not serious, or is somehow the patient's fault. Men who have experienced this pattern often develop what researchers call "medical mistrust" - a reluctance to seek care that persists even after receiving a correct diagnosis.
Acknowledging this history, both to yourself and to new healthcare providers, is an important part of rebuilding a productive relationship with medical care.
Relationships, Intimacy, and Self-Worth
HS affects intimate relationships in ways that are rarely discussed openly. For men, the combination of lesion location, pain, odor, and shame creates specific barriers to physical and emotional intimacy.
Fear of disclosure
Many men with HS avoid new relationships or delay physical intimacy because they do not know how or when to disclose their condition. The fear of rejection is real and often based on past experiences of negative reactions.
Sexual avoidance
Pain, active lesions, and self-consciousness about appearance and odor lead many men to avoid sexual activity even in established relationships. This avoidance, if not communicated, can create distance and misunderstanding with partners.
Identity and masculinity
For men who strongly associate physical capability and appearance with their sense of self, HS can feel like a direct attack on identity. The inability to do physical activities, the visible scarring, and the dependence on medical care can all challenge a man's sense of who he is.
Partner burden and guilt
Men with HS often feel guilty about the impact of their condition on partners - the wound care, the cancelled plans, the financial cost of treatment. This guilt, if unaddressed, can become a source of ongoing psychological distress.
A Note on Disclosure
There is no perfect time or script for disclosing HS to a partner. What matters is finding a calm moment outside of a physical encounter, using clear language ("I have a chronic skin condition called hidradenitis suppurativa"), and giving the other person time to process. Most people respond better than anticipated. The anticipatory anxiety is usually worse than the actual conversation.
Practical Support Strategies for Men
Mental health support for men with HS does not have to look like traditional therapy. There are multiple entry points depending on what feels accessible.
Name what you are experiencing
Depression, anxiety, shame, and grief are not weaknesses. They are normal responses to a painful, stigmatized chronic condition. Naming the experience is the first step toward addressing it.
Talk to your dermatologist about mental health
Many dermatologists now screen for depression and anxiety in HS patients. If yours does not, raise it directly. 'I have been struggling emotionally with this condition' is a complete sentence that opens the door.
Consider CBT or ACT therapy
Cognitive Behavioral Therapy (CBT) and Acceptance and Commitment Therapy (ACT) have the strongest evidence base for chronic illness-related psychological distress. Both can be accessed online if in-person feels like too high a barrier.
Find at least one person who knows
Carrying HS entirely alone is a significant psychological burden. Finding one person - a partner, friend, family member, or online community member - who knows about your condition reduces isolation meaningfully.
Use structured online resources
If formal therapy is not accessible, structured online programs for chronic illness and depression (such as those based on CBT principles) can provide meaningful support. The HS Foundation and patient advocacy organizations also offer peer connection resources.
Address the physical and psychological together
Treating HS medically without addressing the psychological burden leaves half the disease untreated. Advocate for a care plan that includes both. Some academic medical centers have integrated dermatology-psychology programs specifically for conditions like HS.
Reality Check
The psychological burden of HS in men is real, documented, and undertreated.
Shame, silence, and delayed diagnosis are not personal failures. They are predictable outcomes of a stigmatized condition in a culture that discourages men from seeking help.
Addressing the mental health impact of HS is not optional. It is part of treating the disease.
When to Seek Urgent Mental Health Support
If you are experiencing any of the following, please reach out to a mental health professional or crisis service immediately:
- Thoughts of self-harm or suicide
- Feeling that life is not worth living because of your condition
- Complete withdrawal from relationships and daily activities
- Inability to care for yourself or manage basic daily tasks
Crisis Text Line: Text HOME to 741741. National Suicide Prevention Lifeline: 988.
Related Resources
HS and Depression & Anxiety
In-depth guide to the mental health comorbidities of HS
Intimacy and Relationships with HS
Guidance on disclosure, physical intimacy, and relationship strain
Men's HS Hub
All articles and resources in the Men's HS Series
HS Support Groups
Online and in-person communities for people with HS
Frequently Asked Questions
Medical Disclaimer
This article is for educational purposes only and does not constitute medical or mental health advice. If you are experiencing depression, anxiety, or thoughts of self-harm, please consult a qualified healthcare professional. In a crisis, contact the 988 Suicide and Crisis Lifeline by calling or texting 988.
References
- [1]Kurek A, et al. A survey of factors associated with quality of life impairment in patients with hidradenitis suppurativa. Acta Derm Venereol. 2013;93(3):342-346.
- [2]Shavit E, et al. Psychiatric comorbidities in 3207 patients with hidradenitis suppurativa. J Eur Acad Dermatol Venereol. 2015;29(2):371-376.
- [3]Vinding GR, et al. Prevalence of skin disease among 7000 adults from a general population. Dermatology. 2014;228(3):261-265.
- [4]Kimball AB, et al. Two phase 3 trials of adalimumab for hidradenitis suppurativa. N Engl J Med. 2016;375(5):422-434.
- [5]Thorlacius L, et al. Delay in diagnosis of hidradenitis suppurativa is a global problem. Br J Dermatol. 2018;178(6):1445-1446.