HS and Itching: What It Means
Itching is one of the most disruptive and least-discussed symptoms of hidradenitis suppurativa. Understanding why it happens - and what it is telling you - is the first step to managing it.
Itching in HS is not random. It is a direct signal from your immune system, your skin's repair processes, and your environment. Learning to read that signal - rather than react to it - gives you real information about what is happening in your body and what to do next.
Why HS Causes Itching
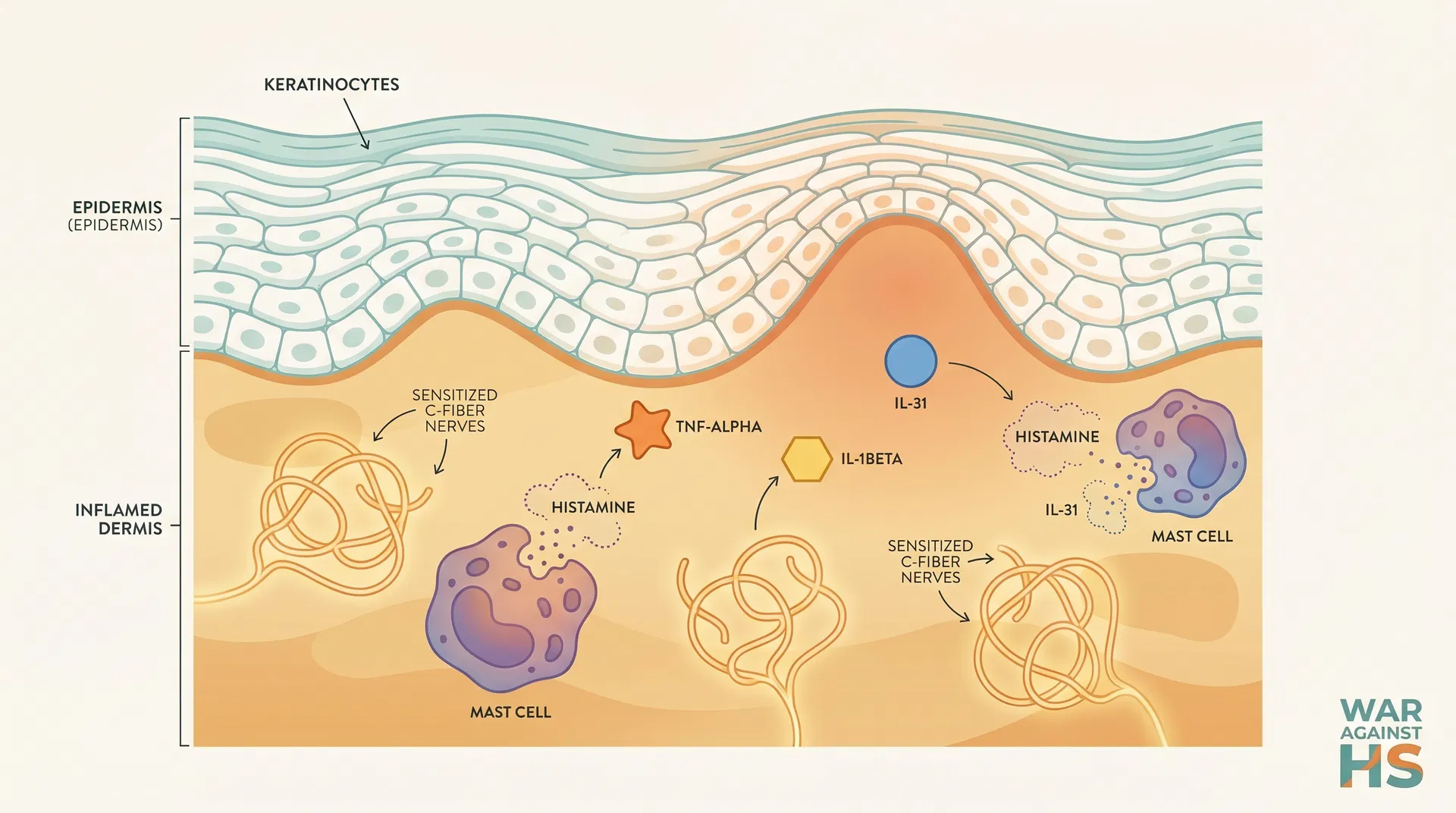
HS itching is not a single symptom with a single cause. There are five distinct mechanisms at work, and they can overlap at any point in a flare cycle.
Inflammation Irritates Nerve Endings
When HS flares, your immune system floods the affected area with inflammatory chemicals like histamine, prostaglandins, and cytokines. These chemicals directly stimulate the itch-sensing nerve fibers (C-fibers) in your skin. The more active the inflammation, the more intense the itch signal your brain receives. This is the same pathway that makes insect bites and allergic reactions itch.
Blocked Hair Follicles and Pressure
HS begins when hair follicles become plugged with keratin and debris. As the blockage builds, pressure increases inside the follicle and the surrounding tissue. This pressure compresses nearby nerve endings, triggering a deep, persistent itch that is different from surface-level itching. It often feels like something is pushing from the inside out.
Healing Skin Itching
After a flare begins to resolve, the skin enters a repair phase. New skin cells grow, collagen is laid down, and the tissue reorganizes. This healing process stimulates the same nerve fibers responsible for itch. If you notice itching after a lesion starts to improve, it often means your skin is actively repairing itself - a positive sign, even if uncomfortable.
Bacterial Activity and Drainage
HS lesions frequently become colonized with bacteria, particularly Staphylococcus aureus and anaerobic species. Bacterial metabolites and the body's immune response to them can amplify the itch signal. When a lesion is draining, the drainage itself can irritate the surrounding skin, adding a secondary itch on top of the primary inflammatory itch.
Sweat and Friction
HS most commonly affects areas where skin folds touch: armpits, groin, under the breasts, and the inner thighs. Sweat in these areas is trapped by skin-on-skin contact, creating a warm, moist environment that irritates already-sensitive skin. Friction from clothing or movement adds mechanical stimulation to nerve endings that are already primed to fire by inflammation.
The Itch-Scratch Cycle
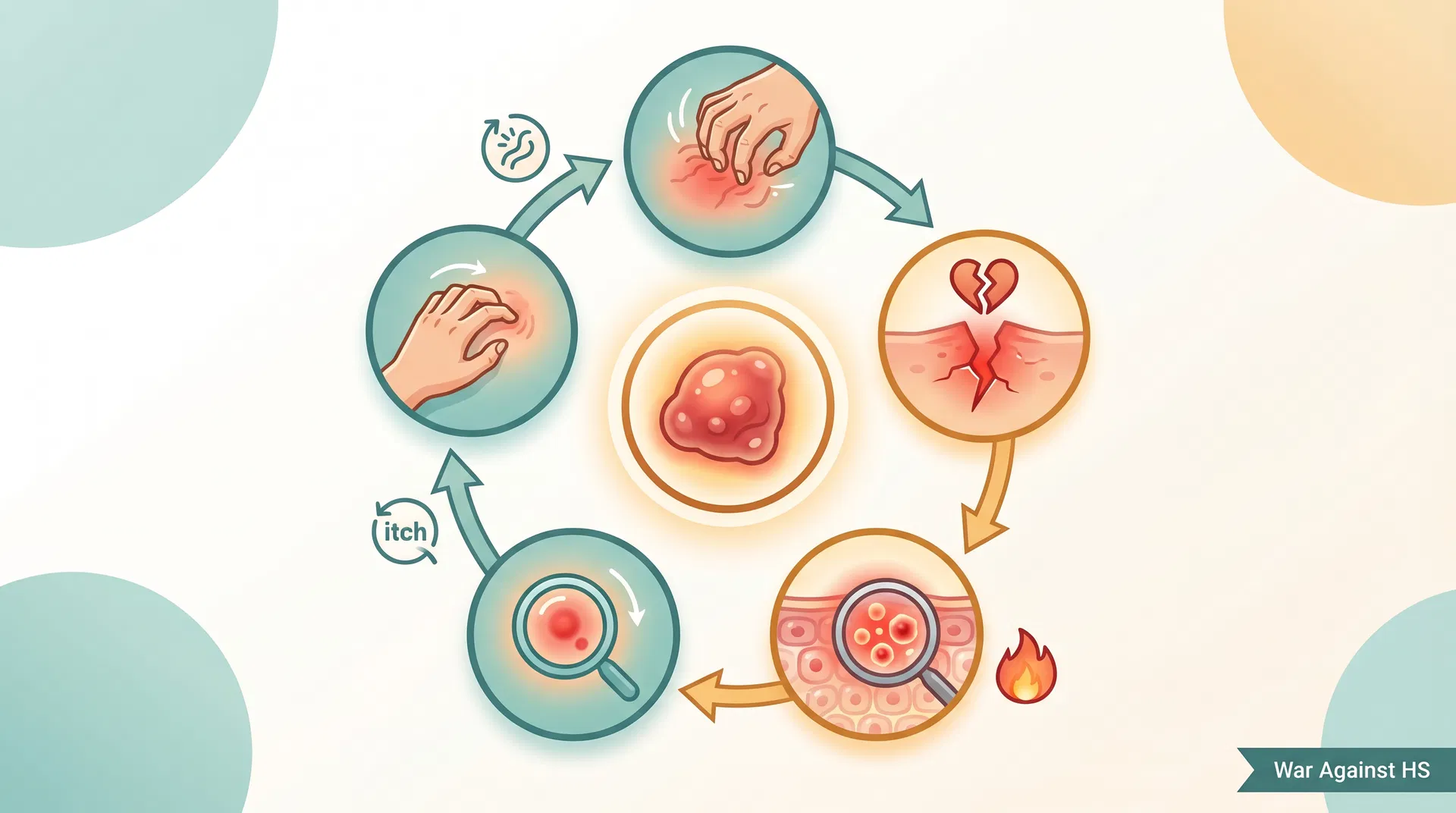
Critical Warning: Do Not Scratch
Scratching an HS lesion feels like relief for a few seconds - but it sets off a chain reaction that makes your HS worse. The itch-scratch cycle is one of the most damaging patterns in HS management.
Scratching an HS lesion:
- -Breaks skin barrier: Creates micro-tears that allow bacteria to enter and increase infection risk.
- -Increases inflammation: Mechanical trauma to the skin triggers additional immune activation, worsening the flare.
- -Triggers lesion formation: Repeated trauma to follicle-dense areas can initiate new HS lesions in previously unaffected skin.
- -Delays healing: Every scratch disrupts the repair process, extending the duration of the flare and increasing scarring risk.
Use a cool compress or gentle pressure instead. The goal is to interrupt the itch signal without damaging the skin.
The itch-scratch cycle is self-reinforcing: scratching causes micro-inflammation, which increases the itch signal, which makes you want to scratch again. Breaking this cycle - even once - reduces the inflammatory load and gives your skin a chance to stabilize.
What the Itching Is Telling You
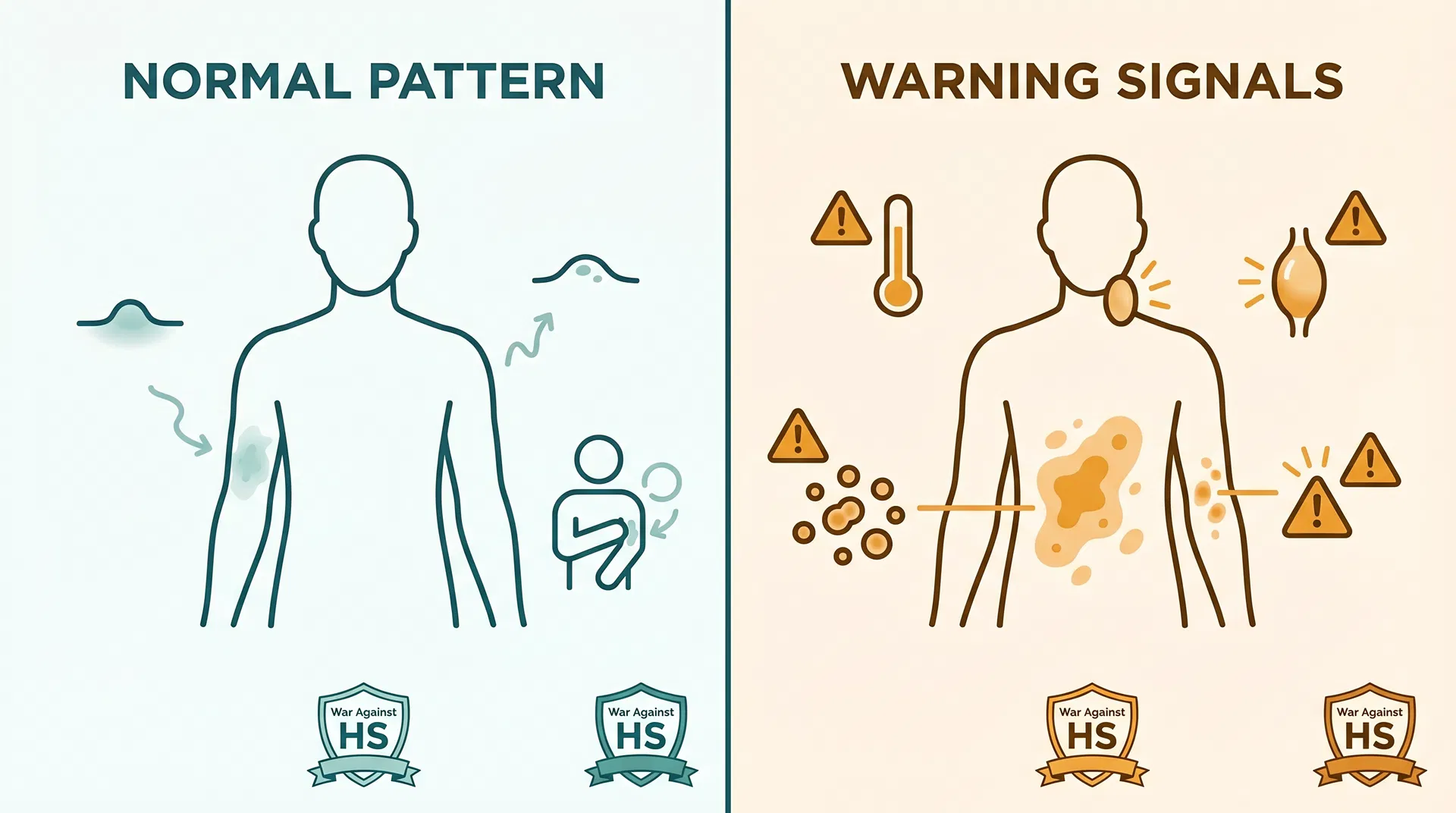
Itching is information. Different types of itch in HS correspond to different stages of the flare cycle. Learning to read the signal helps you respond with the right action at the right time.
Early flare signal
Early WarningItching that appears before any visible lesion is often your body's first warning that a flare is developing. Catching this early gives you a window to apply topicals, reduce friction, and avoid known triggers.
Active inflammation
Active FlareIntense, persistent itching alongside visible redness, warmth, or swelling indicates an active inflammatory flare. This is the peak of immune activity in the area and is the phase most likely to benefit from anti-inflammatory treatments.
Healing phase
HealingA milder, more surface-level itch that follows a flare - especially if the lesion is flattening or crusting - usually signals that healing is underway. This itch is normal and expected. Gentle moisturizing can help manage it without disrupting the repair process.
External irritation
External TriggerItching that appears after exercise, in hot weather, or when wearing certain fabrics is often driven by sweat, friction, or contact irritants rather than a new flare. Identifying and removing the trigger usually resolves this type quickly.
Tracking when your itch appears - and what it feels like - gives you and your dermatologist actionable data. Consider logging itch onset in a flare diary alongside your other symptoms.
How to Relieve HS Itching

Effective itch management in HS works on three levels: immediate relief, targeted skin treatment, and addressing the underlying inflammation that drives the itch in the first place.
Short-Term Relief
Targeted Topicals
Root-Level Control
When Itching Is a Warning Sign
Most HS itching is a normal part of the flare cycle. But some itch patterns warrant prompt medical attention. Contact your dermatologist if you notice any of the following:
- Sudden intense itching with spreading redness: May indicate a secondary bacterial infection or cellulitis spreading beyond the HS lesion.
- A spreading rash in a new area: Could signal an allergic reaction to a topical product, or a new HS lesion forming in a previously unaffected site.
- Nighttime itching that disrupts sleep: Persistent nocturnal itch can indicate systemic inflammation, a new comorbidity (such as thyroid dysfunction or anemia), or a reaction to medication.
This content is educational and not a substitute for medical care. Always consult a qualified healthcare provider for diagnosis and treatment of hidradenitis suppurativa.
Continue Learning
Stay Informed on HS Research
Get the latest HS symptom management strategies and treatment updates delivered to your inbox.